MAT Program for Addiction
Orange County Medication-Assisted Treatment Program
At Renaissance Recovery, our treatment center is proud to announce that we offer Medication-Assisted Treatment Program (MAT) in Orange County, CA. Renaissance Recovery and its respective leadership know that MAT is an effective form of treatment to fight addiction, according to SAMHSA it is proven to improve patient survival and increase retention in treatment.

By: Renaissance Recovery
Clinically Reviewed by: Diana Vo, LMFT
Last Updated:
04/19/2024
What Is a Medication-Assisted Treatment Program?
For people who are still asking “What is Medication-assisted treatment?” let’s get a better understanding. MAT uses FDA-approved medications in conjunction with other counseling and behavioral therapies. This treatment option is overseen by a medical doctor who has received the additional necessary training to treat substance use disorder with the assistance of conjunctive medication.
Research has shown MAT, such as Vivitrol, is a proven, evidence-based form of treatment that can successfully treat these disorders, and can even help people in long-term recovery.
Table of Contents
Understanding Medication-Assisted Treatment
The medications used in MAT will allow your body to more easily go through the withdrawal process and deal with the associated symptoms.
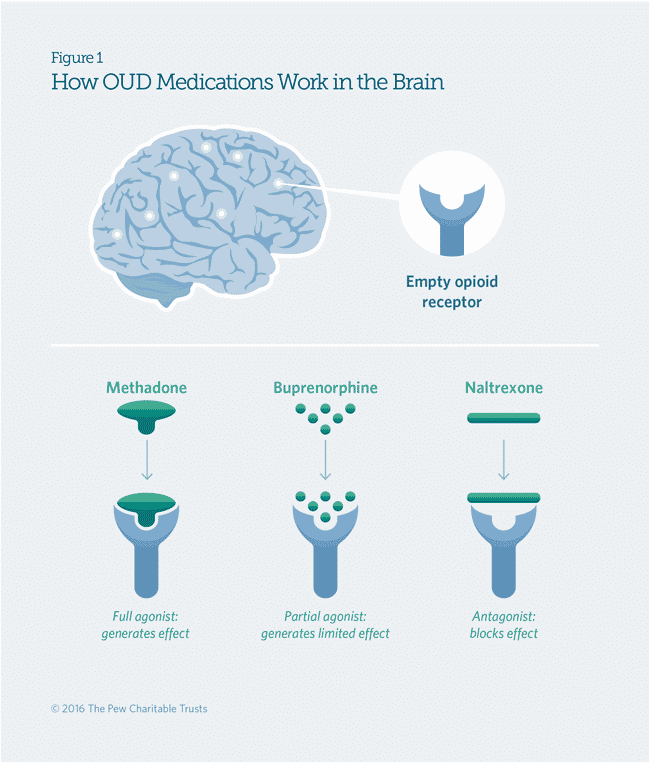
These drugs fall under 3 main categories:
- Agonists: Activate opioid receptors powerfully
- Partial agonists: Milder activation of opioid receptors
- Antagonists: Block the opioid receptors and their rewarding effects
The precise medication used will vary according to your needs.
Among the above groups, the most commonly used of these drugs are:
- Buprenorphine
- Methadone
- Naltrexone
- Disulfiram
- Buspar
Most Common MAT Drugs
Buprenorphine (branded as Subutex or Suboxone) is a partial opioid agonist. It helps to minimize cravings for certain substances without triggering a high. Approved by the FDA in 2002, buprenorphine became the first drug physicians could prescribe under the new Drug Addiction Treatment Act. Approval led to increased access to this treatment.
When taken as prescribed buprenorphine is safe and effective in helping diminish the effects of physical dependence that opioids can have on an individual. While there are side effects associated with buprenorphine use, it can help individuals who are dealing with withdrawal symptoms associated with buprenorphine.
Methadone is a long-acting opioid agonist taken orally under supervision.
The function of methadone use is to reduce opioid craving and withdrawal and blunt or block the effects of opioids. When taken as prescribed, methadone is a safe and effective method to help those who have fallen into an opioid addiction.
Methadone is administered in an outpatient setting.
Naltrexone is an opioid antagonist that interferes with the way opioids act. Neither sedating nor addictive, you can find naltrexone as an injectable, a nasal spray, or an auto-pen.
Naltrexone is not an opioid and is used to block the euphoric and sedative effects that is caused by opioids such as heroin, codeine, morphine, and more.
Current research shows that MAT can be used to treat heroin addiction and opioid use disorder with few drawbacks. Using medication improves overall retention in treatment programs while reducing criminal activity and the transmission of infectious diseases.
A Common Misconception About MAT
A common misconception associated with MAT is that it substitutes one drug for another. However, this is not true. Instead, MAT is used to relieve the withdrawal symptoms and psychological cravings that many experience, making treatment easier. This provides stability for the client so that they can begin the necessary clinical work they need in order to achieve long term recovery.
Buprenorphine, approved for use in 2002 by the FDA, represents the latest advance in MAT. Utilization of Buprenorphine in combination with other treatment modalities provide a whole-patient approach to opioid dependency. Buprenorphine is a partial opioid agonist. An opioid agonist satisfies the body’s craving for opiate, which eliminates withdrawals. However, the main point is that Buprenorphine does not produce the same level of euphoria. Buprenorphine has a “ceiling effect,” which reduces the potential for misuse.
Benefits of Medication-Assisted Treatment Program
There are many benefits to our medication-assisted treatment program in Orange County, CA, including:
- Safety – Medication-assisted treatment is safer than quitting at home because people are under the supervision of trained medical professionals.
- Less chance of relapse – Medications used in MAT can block the effects of opioids in the brain. People don’t get the “high” that they crave, and as a result, are less likely to seek out opioids to abuse.
- Sustained recovery – Because MAT normalizes brain chemistry, people with opioid addictions can truly focus on their treatment plans. As a result, there is a higher chance for people to maintain their recovery because they have a stronger foundation.
- Lower crime rate – Numerous studies have shown that people who complete MAT are less likely to commit a crime and less likely to be incarcerated.
- Cost-effective – Billions of dollars each year are lost due to lost productivity at work, health care fees, and costs associated with the criminal justice system. Medication-assisted treatment has been proven to significantly reduce these costs.

Medication-Assisted Treatment in California
If you are looking for a MAT program in California, Renaissance Recovery’s California rehab can help you. We have a treatment program that provides the full continuum of care, including a medication-assisted treatment program. We are based in Orange County but have connections around the entire Southern California area.
If you are interested in learning more about our Orange County medication-assisted treatment, please give us a call today to discover how we can help you start your new sober life.
Rehabilitation can put an end to addiction
Call and ask the facility directly or call your own provider to determine if your insurance covers the treatment.

